Having just spent my morning getting myself and the girls ready to go to Spina Bifida Clinic, three hours and change trapped with two two-year-olds in one exam room, and having gotten them home without car napping and successfully into and asleep in their beds, I pondered a daytime adult beverage. Instead, I wrote a blog post. Continue reading “A Claire Update”
graduation day

I interrupt my regularly scheduled ramblings to bring you a moment of shameless bragging on my husband. Tonight, we will celebrate his very last graduation in what has been a very arduous journey toward his medical career. 4 years of college. 4 years of medical school. 3 years of residency, followed by boards. And now 3 years of fellowship, coming to an end, in which he will be board certified in pediatrics and pediatric emergency medicine, and on Monday will officially begin work as an attending physician, or, even more specifically and rad, an Assistant Professor of Pediatrics, in the emergency department.
Last night, as we sipped some wine, I told him, “I’m so proud of you for finally being finished.” He asked if I had to throw the “finally” in there, but I maintain that the “finally” is necessary to indicate just what a long, difficult process this has been. I wish I could do the math on all the hours spent working and studying to get to this place. I have never seen anyone work harder to achieve their dream, and what a beautiful dream to want to take care of the tiniest patients and help them to be healthy and feel safe. As I tell people, you don’t want to have to take your kid to the ER, but if you do, he will take GREAT care of you.
I’m excited for this next step in Jon’s career and for our family, and I am so very happy and proud.
Claire is doing great
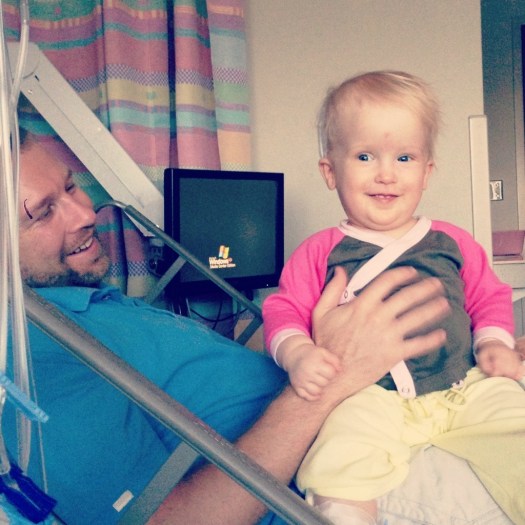
Just woke up from as good of a sleep as one can hope for in a hospital, cuddling my Claire Bear all night. She came through surgery like a champ, waking up happy after anesthesia, and generally being the most chilled out kid who just had brain surgery anyone has ever seen. Her surgeons say everything went great, and judging by the pressure her cerebral spinal fluid was under, it really was time for us to do this VP shunt. She probably has been having a headache from the pressure lately and we didn’t even know it. Now, her head should stop growing so quickly and the rest of her should catch up.
We’re super grateful for the excellent care we’ve been getting, as well as all the love and support from folks like you. It looks like we will go home this evening.
A Claire Bear update: neurosurgery on Monday
 We just got back from a visit with our (much loved) neurosurgeon, and based on new information in last week’s MRI, we have decided in consultation with her and another neurosurgeon she asked to give a second opinion, that it’s time for Claire to get a shunt placed to treat her hydrocephalus. The lay explanation is, due to her spinal defect and chiari malformation, Claire’s cerebral spinal fluid doesn’t drain from her head and spine properly, causing fluid to build up in her head (aka hydrocephalus). While she has had the hydrocephalus from the start, we and our surgeon chose to take a conservative approach instead of operating when she was a wee baby, because surgery is always risky, because the risk of infection and complications is greater in younger babies, and because clinically, she was having no symptoms or problems from the hydrocephalus other than a big head as a result of the fluid buildup.
We just got back from a visit with our (much loved) neurosurgeon, and based on new information in last week’s MRI, we have decided in consultation with her and another neurosurgeon she asked to give a second opinion, that it’s time for Claire to get a shunt placed to treat her hydrocephalus. The lay explanation is, due to her spinal defect and chiari malformation, Claire’s cerebral spinal fluid doesn’t drain from her head and spine properly, causing fluid to build up in her head (aka hydrocephalus). While she has had the hydrocephalus from the start, we and our surgeon chose to take a conservative approach instead of operating when she was a wee baby, because surgery is always risky, because the risk of infection and complications is greater in younger babies, and because clinically, she was having no symptoms or problems from the hydrocephalus other than a big head as a result of the fluid buildup.
However, the MRI we got last week showed that not only are the ventricles in her head very large, indicating a lot of fluid has built up there, but also she has developed a syrinx, or pocket of fluid within her spinal cord. This has the potential to cause her to have problems with her arms and legs, and given the great strides and progress she has made mobility wise, and the hope we have for continued progress, we do not want to risk this syrinx compromising her physical abilities in any way.
It is for these reasons that we’ve agreed to have the shunt placed on Monday morning. We are of course a little disappointed that she has to have neurosurgery, but we are ultimately confident that this is the right time, and hopeful that taking this step now will give her the greatest chance to achieve all she can developmentally. She’ll stay one night in the hospital, and then should be back to her normal activities within a week or two. Thanks for always cheering Claire on– her internet fan club means more to us than you can know.
Awareness
I found out today that October is Spina Bifida Awareness Month. My first thought was: what a crap choice in awareness months. I mean, everyone knows that October is Breast Cancer Awareness Month, as pink has pretty much blanketed everything we see.
But then I thought, well, it’s just as well, since I’m generally skeptical of “awareness” in general. I mean, I’m not usually sure of what it accomplishes. Half of the pink I see this time of the year seems to have no real point, as most of us are aware that breast cancer exists, and the pinkwashing is often unaccompanied by anything about breast exams or early detection or risk factors or anything.

I guess people are less aware of the realities of spina bifida. SB is a congenital defect of the “neural tube” which is the part of a fetus that eventually becomes the baby’s head and spine. Claire’s neural tube didn’t close properly, and when she was born, she had 4 centimeters of her spine visible from the outside. As a result of this defect, things like nerves weren’t hooked up properly, so she has/will have certain amounts of disability in her legs, bladder, and bowels, in addition to hydrocephalus, or fluid building up in her head (which for many people with SB requires surgery to place a shunt and drain the fluid, though we haven’t had that yet). While her spinal defect was one of the more severe types, she seems to have good enervation and musculature in her legs, and her doctors and physical therapists believe she will walk and will only need braces to support her ankles, though some people with SB require more extensive bracing or even use wheelchairs.
I certainly didn’t know all of this or really much about SB at all, and it really wasn’t even on my radar until my birthday last year, when we went in for a 20 week ultrasound, excited to finally learn our babies’ sexes, and instead learned that the baby we’d later name Claire had SB. It was a really scary, sad day.
But the thing I needed awareness of that day wasn’t just “spina bifida” as some vague concept. I needed to be aware of the beautiful reality that would be my daughter’s life. Yes, we both had a rocky start. She had surgery at two days old. She was separated from me for 9 days. She was in the NICU for two weeks. She had to stay on her belly for 6 weeks while her back healed. But despite all of that, she’s really just a baby. They’re all very needy. They’re all very fragile. They’re all very tiny. They’re all amazing little creatures. If you looked at my two girls today, you might not be able to guess which one has SB.
If I could go back to last December 16 and make myself aware of anything it would be this: Claire is beautiful. She is funny. She is sweet. She has a radiant smile. She loves to eat. She loves her mama and daddy. She is exploring and learning and growing every single day.
I was so worried about all the ways she’d be different from her able-bodied twin sister, but the reality is, they’re both just babies. They are completely different and yet so very much the same. And almost all of my worrying was completely unnecessary. That is what I needed to be aware of: that there was nothing to be afraid of.
So, no, you likely won’t see NFL teams raising awareness for SB this month, or yellow covering all your favorite products in the name of raising funds. And while you may not personally know anyone affected by SB, now you know a little more about our story, and a little more about my baby Claire, who is special, just like everyone else.

Claire update: no surgery this week
 After seeming to talk us into the shunt surgery in the ER, our neurosurgeon seemed to spend our clinic visit talking us out of it. While she seems to agree that the surgery is basically inevitable, there is still a slim slim chance the hydrocephalus will arrest, and since she’s not having severe symptoms at this time, we have a little time to wait. In the meantime, we’re probably going to start her on Zantac and see if that helps the vomiting.
After seeming to talk us into the shunt surgery in the ER, our neurosurgeon seemed to spend our clinic visit talking us out of it. While she seems to agree that the surgery is basically inevitable, there is still a slim slim chance the hydrocephalus will arrest, and since she’s not having severe symptoms at this time, we have a little time to wait. In the meantime, we’re probably going to start her on Zantac and see if that helps the vomiting.
I’m glad this means no surgery this week, though I’m pretty sure she will need the shunt at some point. Guess we’ll be staying in style when that happens, because the new infant and toddler unit at our children’s hospital will be open by then.
I also realize I haven’t updated about MY health issues in a while. Based on my slow recovery and echo-cardiograms, my cardiologist had me do a contrasted cardiac MRI. It was kind of crazy to actually feel the contrast get warm in my chest every time the MRI machine was on, and I now totally see why claustrophobic people totally wig out in those things. Personally, I pretended I was an astronaut about to be blasted into space. Anyway, the upshot is, it looks increasingly like I have a congenital heart defect called left ventricle non-compaction syndrome, which basically means the tissue in my left ventricle didn’t form correctly, which is why it’s weak and has such a “poor squeeze.” The strain and stress of the pregnancy on my body is what finally made my condition severe enough to notice. I now feel vindicated and want to go back to every PE teacher I ever had and explain that my poor performance in everything endurance related is actually the fault of my heart.
The MRI also showed that my ejection fraction (a measure of how well the heart pumps blood into the body) has improved from 15% to about 30% (normal is still 50% or better). I’m still doing well on my ever-increasing cocktail of meds, and I think my doctor will be adding a third medicine (I’m already on a beta blocker and an ace inhibitor) this week, and I hope the transition goes well.
Anyway, that’s what’s going on with Claire and me health-wise. Thank you again for all of your support, thoughts, and prayers.
surgery for baby claire
 Last Thursday we spent most of the day in the ER with Claire, because her already more-than-average spit up had become projectile vomiting in the last couple of weeks, and had escalated to every other feed or so in the last few days. Dr. Dad thought she might have pyloric stenosis, and additionally, since increased vomiting is a warning sign that her hydrocephalus (extra fluid in her head because of the way her spinal defect pulled down her spinal cord and blocked the exits for the cerebral-spinal fluid) is getting more severe, so we wanted her to get worked up.
Last Thursday we spent most of the day in the ER with Claire, because her already more-than-average spit up had become projectile vomiting in the last couple of weeks, and had escalated to every other feed or so in the last few days. Dr. Dad thought she might have pyloric stenosis, and additionally, since increased vomiting is a warning sign that her hydrocephalus (extra fluid in her head because of the way her spinal defect pulled down her spinal cord and blocked the exits for the cerebral-spinal fluid) is getting more severe, so we wanted her to get worked up.
She got an ultrasound of her pyloris, which ruled out pyloric stenosis, so she got an ultrasound of her head, which revealed more fluid in the ventricles of her head than the last time we looked. She also got a head CT to get an even clearer picture. Her neurosurgeon, whom we love, insisted on coming down from clinic to see “her girl” personally, and we discussed whether or not it’s time to move forward with surgery to place a shunt that would drain the excess fluid from her head into her belly where her body could then absorb and deal with it.
The bottom line is, it looks like it’s time to get the shunt surgery. We had been hoping to avoid it, but we think that since the fluid continues to increase, we’d rather go ahead and do something about it instead of waiting for things to get worse, which would involve symptoms like trouble breathing and swallowing.
We hate that our wee girl has to have surgery again, but we know she’s a trooper and will come through great. We see the neurosurgeon again on Monday morning, and it looks like the surgery will be Tuesday or Wednesday. Not sure how many days inpatient would be involved, yet. Please keep our Claire Bear in your thoughts and prayers, and us too.
a birth and near death story
Some folks may be wondering, since my last post over a week and a half ago was OMG ONE DAY TIL BABIES LET’S FINISH THE NURSERY, whether or not I did in fact have those babies.
I did.
And what a crazy story it is.

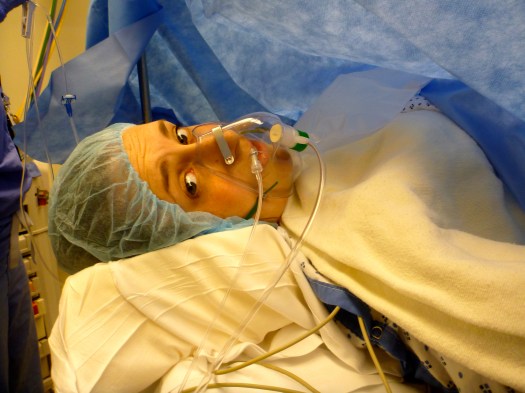
Things started out as planned– we didn’t sleep at all the night before from excitement, and we showed up at the hospital at 7:00 am on Wednesday, March 28 (exactly one month before my 40 week due date) for a C-section that had been moved up 5 days because I suddenly had an elevated blood pressure and had started retaining fluid. I was really nervous about the surgery, but despite a little trouble getting the spinal/epidural combo in place (apparently folks with scoliosis and an extra vertebra are a bit challenging for anesthesiologists), the whole operation went very smoothly. It’s super surreal to be lying on a table, numb from the waist down, knowing you’re being cut open and having babies pulled out, but feeling nothing but pressure and tugs and then suddenly hearing cries. I’m pretty sure I was saying “I’m afraid I’m going to feel it!” to the anesthesiologist who was standing next to me as I was already being cut open.
It turns out my girls, who had been in “bunk beds” or in the transverse position for my entire pregnancy, had turned breech somewhere between my last appointment and the surgery– so I’d have definitely needed a C-section even without my blood pressure issue or Claire having spina bifida. Jon joked afterward that there are about 5 ways I could have died in childbirth this week if not for modern medicine– breech twins are one of them. Jokes aside, there is no one more supportive and awesome than my husband, who was right by my side for the whole surgery. The surgical team kept telling him when to pull out his camera for a good photo op, but he mostly focused on supporting me and keeping me calm. He did have the anesthesiologist give me some “goofy juice” at the end when I started to freak out a bit that I might be feeling more than just pressure (pretty sure that was mental), but overall, he kept me relaxed.

After both girls were pulled out, Etta weighing 6.2 lbs. and Claire weighing 6 lbs. (I am SO FREAKING PROUD of those weights for 35 weeker twins, I must say), Jon went with the babies to the resuscitation area, which sounds scary, but doesn’t necessarily mean the babies are getting like, CPR or anything. They were checked out by a team of neonatologists and pediatricians, and there was a transport team standing by ready to take Claire from the university hospital where I was delivering to the nearby Children’s Hospital (where my husband works), where she would be having surgery to repair the opening on her spine caused by her spina bifida.
It turned out that Claire’s spinal defect was both higher and larger than we initially hoped. I got to see my baby girl in a plastic transport box for about 5 minutes in recovery before she was whisked away by the transport team. I’m pretty sure the “goofy juice” is what helped me not completely freak out over not getting to hold one of my babies, but we had also prepared ourselves for the fact that this is what would happen on delivery day, knowing it would be happening since week 20 of the pregnancy. I was also very thankful to have met and consulted with the team of doctors who would be taking care of her, so I knew she was in the very best of hands.
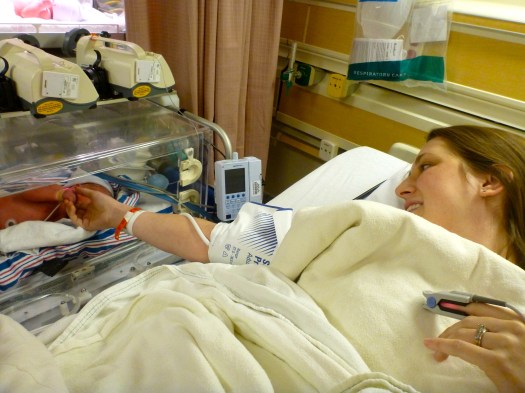
After recovery, Etta and I were moved to the peri-partum ward, and she was allowed to share a room with me. My blood pressure and heart rate were slow to go down, and labs revealed my blood counts were very low, so on Thursday I received a blood transfusion. Everyone who came in the room and saw me afterward remarked on how much better I looked, and the color in my face, even though I was about the same shade as the beige hospital blanket that covered me. I guess I was white as the sheets before?
On Friday, Claire had her surgery, a five hour process involving neuro- and plastic surgeons to cover the 4 cm. area where you could literally see her spine. I wished so desperately that I could be there for her, but was still not in shape to be discharged from the hospital, so a social worker set up a video-conference and I got to video chat with her before the operation. She opened her eyes when she heard my voice, which made me feel so much better that she still knew her mama loved her. She came through the surgery great, and continues to recover in the NICU at Children’s. She seems to move her legs of her own accord and also to respond to stimuli, which are great signs that she may not have disability in her legs. As with everything, though, we will just have to wait and see. She may also have disability in her bladder and bowel functions, but since no babies have bladder and bowel control at this point, we won’t know until she’s older if this is the case. We certainly hope it isn’t.
On Saturday, there was talk of discharging me from the hospital as I was doing much better, but I was still feeling very very weak and not very able to get out of bed, and when my doctor suggested keeping me another day, I said I thought that was a good idea. I needed the time to continue to recuperate.
By early Sunday morning, I was feeling well enough to get out of bed and walk unassisted the 5 steps to the bathroom, as Jon was holding Etta. I remember feeling so proud as I stood up and walked unassisted, thinking this was finally the milestone I needed to get to go home. As I walked back to the bed, I felt myself getting shorter and shorter of breath. I told Jon I was having trouble breathing, and he called for the nurse. It just got worse and worse, as I struggled for breath in short gasps, and a crowd of nurses gathered around. People were telling me to take a deep breath, but short gasps were all I could manage. I began to hear crackling in my lungs (Jon later explained that this was flash pulmonary edema), and I became more and more panicked. I knew from the way I felt and the look on Jon’s face that I was crashing.
The Rapid Response team arrived and soon I was being prodded and various breathing masks were being shoved onto my face, which only increased my feeling of panic. I know enough from being raised by medical professionals and married to an emergency physician that I needed to be intubated. I was looking at Jon begging him with my eyes to get someone to sedate and intubate me so I wouldn’t have to panic and struggle to breathe any more. From the look on his face, I could tell if he’d had a cart nearby, he would have done it himself. I truly believed I was dying, lying in that bed, surrounded by people bustling around to save me, with my husband watching and my baby girl lying next to me in a bassinet.
And then I don’t remember anything.
My next memory is vague, like a dream, where you know there is something you MUST do, and in this dream, what I had to do was pull something out of my mouth. So I just kept pulling.
It was Monday morning, and I had extubated myself. I was in the ICU, where I had spent about 24 hours on a ventilator.
After consults with cardiologists and pulmonologists and internal medicine specialists and more doctors than I can count, it seems I have developed peri-partum cardiomyopathy, which was causing congestive heart failure. My terribly lay understanding is that possibly due to the stress of the pregnancy on my body, I either developed or finally exhibited a pre-existing weakness in the muscle of my heart, specifically in the last chamber (left ventricle) that sends blood out into the body. The ability of this chamber to pump out blood effectively is measured in an “ejection fraction.” Most people’s is 50% or better, and mine was 15%.

Putting me on the ventilator helped them pump fluid out of my body to take the load off my heart and lungs. They removed 7 liters of fluid from my body in my 24 hours in the ICU, and continued to take more off through diuretics and fluid restrictions after they got me out of the unit and back in the peri-partum ward.
Tuesday through Thursday were spent trying to fine-tune the cocktail of medicines I am now on to control my heart rate and blood pressure and allow my heart to strengthen and heal. Every day they tweaked the meds a bit, and every day I worked harder to get out of bed and walk and move. By Wednesday night, I finally was able to make half a lap around the ward, pushing Etta in a bassinet, Jon beside me to steady me, with nurses cheering– even those who hadn’t cared for me had heard about the girl who was seemingly ready to go home and had suddenly crashed and wound up in the ICU on a vent, so they were proud to see me looking better.


At first, the medicines made me feel worse, which my cardiologist told me would happen. I’d get my meds, and then for 4 hours afterward, feel hot flashes and jitters and general exhaustion, only able to sweat and sleep. But every day that got a little better. By Thursday, Jon and me, and Etta, if I may speak for her, were just DONE being in the hospital. Convinced that I would be compliant with my meds, diligent in home blood pressure checks, and sure to come back for follow-up treatment, I was finally discharged. I have never been so glad to breathe fresh air as when baby Etta and I were wheeled out to the curb in front of the hospital on that beautiful spring day when we finally got to go home. I’m feeling better and better since then. My heart condition may never be fully cured, but it can get a LOT better, and I have high hopes of being one of the successful cases. We will not be able to have any future pregnancies, however, because it would literally mean risking my life.
Another loss that I feel very deeply is the loss of the ability to breastfeed the babies. I had really hoped to be able to nurse them, and had been working on nursing Etta and pumping and building up my supply while in the hospital, however, after the whole almost-dying thing, my doctors convinced me that breastfeeding is a major physical strain on my body, and I needed to be conserving my physical resources to give my heart the best chance to heal, so that I could become strong enough to care for my girls. I have cried many tears over this loss, but I know that we made the right choice for our family. They need my beating heart a lot more than they need breast milk.
We’re still missing 1/4 of our family, with Claire still in the NICU, and we are anxious to get her home. I’m still pretty weak, though stronger every day, and my one outing a day is to go visit her. Blessedly, Children’s has a special “twin rule” that lets us bring Etta with us to visit her sister, and it’s super special just to have the four of us together for a little bit each day– giving us a taste of how great it will be to finally have all of us home. We don’t have a specific date that she’ll be discharged, but we hope it could be soon if she keeps meeting the goals her doctors set for her. Every day that I’m wheeled out of that NICU with only one baby feels incomplete.
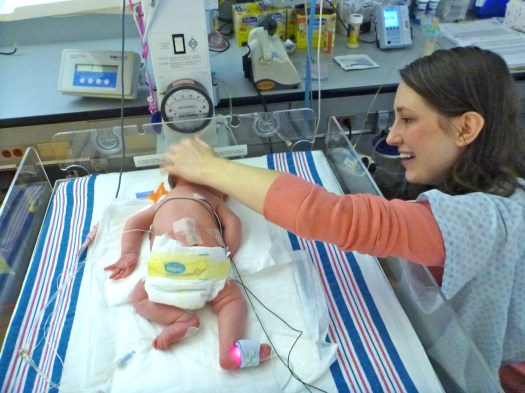

Overall, though, I am so very thankful. I’m glad I was in the hospital where I could quickly get the care I needed when I crashed. I’m glad Claire has such awesome people taking care of her, and glad we have awesome families who would come and take care of her and Jon and Etta and me when we needed them. I’m thankful for two beautiful baby girls. I’m thankful to be alive.

guest post: Jon’s trip to Haiti
My husband Jon was recently part of a team that went to Haiti to run clinics. Since many of this blog’s readers supported the trip financially and through prayers, I thought you might like to read about the trip in his words. Here’s his story:
I have no idea how to best convey what I saw and experienced in Haiti. Had this been my first experience in a 3rd world country, I believe I would have been balled up crying after the first day. I have seen dire poverty before, but nothing close to what I saw in Port-au-Prince. Really, unless you personally go there, it is impossible to get an idea of what is going on. But I will try to paint a picture.
 The enormity of the problem and the reality of the hundreds of thousands of displaced Haitians hit home on our approach to the Port-au-Prince airport. Looking out over the city, as far as I could see were tiny tops of “houses.” By this I mean strung tarps mixed in with battered, rusted tin roofs. At that point, the discussing and planning mode instantly changed into a “oh my gosh, what have I gotten myself into” mode. I was also afraid of what demands customs would make of us to get our medications through customs, but our translator Chris ended up finding a customs agent who knew one of the doctors he worked with in Haiti, and he allowed us to walk right through customs without even a peek into our bags. Hurdle number one jumped.
The enormity of the problem and the reality of the hundreds of thousands of displaced Haitians hit home on our approach to the Port-au-Prince airport. Looking out over the city, as far as I could see were tiny tops of “houses.” By this I mean strung tarps mixed in with battered, rusted tin roofs. At that point, the discussing and planning mode instantly changed into a “oh my gosh, what have I gotten myself into” mode. I was also afraid of what demands customs would make of us to get our medications through customs, but our translator Chris ended up finding a customs agent who knew one of the doctors he worked with in Haiti, and he allowed us to walk right through customs without even a peek into our bags. Hurdle number one jumped.
No matter where or when you drive in Port-au-Prince, the streets are overflowing with people walking, motorcycles zipping through tiny spaces, buses, tap-taps (any kind of large, brightly painted vehicles available for transportation, and you ask to get off by tapping, get it?), merchants and cars, making for a loud, exciting time. The one thing there isn’t a lot of is traffic laws. Who knows what the laws are, there are no lines on the roads, few stop signs and few lights. It’s a miracle there aren’t more accidents. Also, in the streets is all kinds of rubble. Yes, it has been over 18 months since the earthquake, but rubble is everywhere, and even the presidential palace and great cathedral remain in ruins. According to those who live there it is much better than after the earthquake, which I believe, but it was still overwhelming. There were even many partially collapsed buildings that were empty, and probably haven’t been searched for bodies due to the danger of collapse while searching.

On day 2, we finally got to run a “clinic.” We met with Dr. Jeudy, a friend of our hosts, who is in the process of building a new hospital/operating room. We met in his current office, with two crampeded exam rooms, a crowded waiting room, pharmacy and lab on the first floor, an operating room and two large rooms he’s using as inpatient wards on the second floor and living quarters for nurses, as well as a room he sometimes sleeps in on the third floor. He and I saw and admitted a woman with severe pneumonia and respiratory distress before heading to his new site that consisted of concrete floors and some walls where he’s building a new office. We hadn’t advertised the clinic, as he was afraid we didn’t have enough medication, so he told me, “we’ll see people as they come, they’ll probably trickle in, and we’ll start with a slower day.” Ha. As soon as we set up, we were flooded with patients, and between me, him, and a couple ofmedical students, we saw over 270 patients before we had to shut down and turn people away due to impending darkness.
Speaking of darkness, currently in Port-au-Prince, electricity is available for 12 hours a day, and I can only assume it’s some guy’s job to turn off the power. On about half the nights, about 30 minutes after the electricity went off (about 8pm), the power went back on for the night. When it came back on, a loud raucous roar could be heard throughout the city, celebrating a few more hours of light. Some early mornings (like 4am) also consisted of a loud singing/dancing/parade type thing that we were told was a voodoo celebration. Didn’t check it out, but we were all curious.

We ran 5 more busy days of clinic, 2 more in the city, and 3 on the outskirts of town. We mainly saw headaches, abdominal cramps, menstrual cramps, reflux, pneumonia, yeast infections, ear infections, colds, arthritis, high blood pressure…much like you would see in a primary care clinic in the States. However, nobody had glasses (probably accounted for many headaches) and they couldn’t afford to buy pain relievers, cough syrup or antacids. We gave all the kids tooth brushes and many of them vitamins, and presumptively treated worms, malaria (for anyone with high temps and flu-like symptoms) and cholera (all severe GI symptoms.) While running a clinic in the schools, I saw a child with epilepsy who had already seen a doctor, who had recommended seizure medicines, but she could not afford them. We didn’t have any medication for that either, so had to just give advice: don’t swim, drive cars, climb trees, etc. and support the airway when she had seizures. Very frustrating not to be able to treat, but we couldn’t take everything with us. We also saw several kids with mumps (I hadn’t seen that before), measles, and lots of tinea capitis (ringworm on the scalp). I sent one dehydrated, lethargic 11 day old to the hospital for care we couldn’t give, and kept one 4 month old in the clinic for a couple hours to hydrate orally when we found him to be lethargic with a >200 heart rate. He seemed to perk up after fluids! One older lady had stepped on a rusty nail, and was beginning to show signs of tetanus-I excised the wound, started her on Flagyl and told her to find a hospital for further care.


While brainstorming about ideas to help this poor country, we discussed different things people have tried, but lead to further problems, often due to the Haitians’ hand to mouth living situation, a situation created, nurtured, and sustained by the West since the colonial days. One example: Although there are chickens and goats roaming free everywhere, all the chicken, eggs and goat’s milk you buy in Haiti is imported from the US. When one group took small laying hens to the country to try and set up an egg farming operation, they explained that the people shouldn’t eat the hens, because they would provide many eggs, they returned the next week and found the hens were all eaten. This may sound crazy, but it’s understandable that people with no idea where their next meal is coming from might prioritize short term relief over a long term solution that may or may not work out. After the earthquake, many Non-governmental organizations came to town to provide free medical care. The people came in such numbers that many local hospitals could no longer stay open, as people no longer wanted to spend money on medical care because they could get free care from the NGO’s. Some aid creates more harm than good, because it prevents local, sustainable solutions from becoming viable.

Due to US trade embargoes placed on Haiti due to coup-de-etats, multiple factories shut down, leaving the workers jobless. It seems that no matter what is tried, there is an opposite reaction that minimizes or reverses the impact that you’re trying to achieve. It’s a very frustrating mind game for sure. The island is beautiful, it’s in the Caribbean, and would have lots to offer if things turned around some, but getting there is difficult.
So, the trip was gratifying, knowing we provided a small amount of medical care to those who would have gone without, but frustrating, seeing vast need going unmet for a majority of Haitians. It is going to take many smart people, lots of money and a long time to reverse both the damage done within a few minutes of time with the earthquake, and the problems created by generations of Haitians living day to day, not knowing where their next meal will be, nor where they will sleep that night. The only lasting solutions will be ones that empower and involve workers, not through hand-outs and band-aids, but through sustainable programs that allow Haitians an active role in the repair and renewal of their nation.
it’s outta my hands

At some point in toddlerhood, it eventually hits all of us, the “I can do it by myself!” And from that point on, to be human is to want to be in charge of ourselves. You’re not the boss of me! I choose my choice! I’m in charge!
Lately, though, I find myself feeling like a toddler, trying to DO IT BY MYSELF, and this thing called life keeps reminding me that I’m not always the boss of me, I don’t always get to choose my choice. Boy oh boy does the medical education system that owns our lives right now make that clear. You see, in three weeks, Jon will get an email that will suddenly reveal what we’ll be doing with our lives for the next three years. And it’s more than driving me nuts. Continue reading “it’s outta my hands”